|
This is a copy of a new piece written by Dr Talitha Ford and myself - republished from the original post on Medium. Mental illness is one of the leading causes of disability, and roughly 45.5% of the Australian population is affected by a psychiatric condition at some point in their lifetime.
Psychiatric conditions like schizophrenia, bipolar disorder and autism are typically life-long, but for some people the associated symptoms can be well managed with common drug and psychological therapies, as well as a supportive environment. For others, these symptom management options are less effective, which makes them very much “trial and error”. This is problematic because a delay in effective treatment can lead to more severe deterioration and a greater impact on daily functioning. One possible reason that certain groups of people don’t always respond to first-line treatments for a given condition might relate to the way that the condition itself is diagnosed. Ineffective or incorrect diagnosis can lead to a patient being prescribed treatment that does not specifically address the set of symptoms that uniquely affects them. Symptom variation There is a huge amount of variability in symptoms within any single psychiatric condition. This is partly because the manuals that psychiatrists use to identify and diagnose patients define psychiatric conditions based on a fairly broad set of criteria — for any one condition, a diagnosis is given when the patient meets any number of criteria related to the nature, severity, duration and impact of specific symptoms. Within these criteria, though, there may be many possible combinations of symptoms. And each of these symptoms can vary in severity from patient to patient; in fact, milder symptoms are actually observable in the healthy population as symptom traits at the less extreme end of the symptom spectrum. Because there is no clear cut-off for a “clinically significant” presentation of symptoms, each diagnosis is made through the interpretation of a clinician, which is in itself problematic, given the subjectivity of this approach. Take schizophrenia as an example. A person receiving this diagnosis must have experienced any two of the following five symptoms with an obvious impact on functioning over a long duration: 1) hallucinations (visual or auditory), 2) delusions, 3) disorganized speech, 4) disorganized behaviour, or 5) so called “negative symptoms”, such as social withdrawal or the absence of emotional expression. Only one of symptoms 1, 2 or 3 needs to be present for a diagnosis of schizophrenia, so one person with this diagnosis could have a completely different symptom profile to another. It’s also possible for someone to present with several symptoms that are not deemed clinically significant in terms of severity, and miss out on a diagnosis and the associated support altogether. Separating psychiatric conditions Another complicating factor is that the tools used to diagnose psychiatric conditions were built on the assumption that different psychiatric conditions are, on the whole, independent from each other. That is, the defining symptoms of one psychiatric condition are not assumed to overlap with others . This is like saying that Superman and Spiderman are superheroes because they have superhuman powers, but that Batman isn’t because he’s just a regular guy in a cape. Obviously there are similarities and differences between these characters, but their categorisation as superheroes really just depends on how the criteria are defined. Pigeon-holing symptoms into rigid diagnostic categories is problematic in psychiatry because it also affects the way scientists conduct research — which has so far been mainly focused on investigating conditions as independent and one dimensional. But newer lines of research are beginning to show substantial similarity in genetic risk factors and brain abnormalities across several conditions including autism, schizophrenia, bipolar disorder, major depressive disorder and attention deficit-hyperactivity disorder, which might explain some of the overlapping symptoms between them. Mild non-clinical autistic and schizotypal characteristics have also been closely related in many studies. Not surprisingly, many people actually meet the criteria for more than one psychiatric condition, and some people show combinations of symptoms that don’t fit neatly into any one diagnostic category. In combination, these factors make it very difficult to identify how to best provide care for different individuals. Changing research practices Because of the variability within psychiatric conditions, and the overlap between them, traditional research approaches that focus on understanding broad diagnostic categories aren’t particularly effective for identifying the biological causes of specific symptoms. But focusing on understanding specific symptoms that crossover between people diagnosed with different psychiatric conditions can help to remedy this. Understanding biological causes is critical for the development of new neuroscience-based biological treatments. Despite a refocusing of research priorities, there has been little change within clinical practice. For example, despite the known symptom similarities between autism and schizotypy in children, diagnosis of only one condition is typically made and treatments prescribed accordingly despite not necessarily proving effective. This current practice is troubling because interventions tend to treat a diagnostic category, rather than an individual’s specific combination of symptoms. The consequences of this is the potential to over-treat some symptoms, while under-treating others. Ultimately, the clinical and research community must work together to improve our understanding of psychiatric conditions, especially to pin-point the biological and brain processes that may cause common, overlapping symptoms. This will allow for the development of more effective treatment options that will improve the lives of those who struggle with these symptoms, regardless of their given diagnosis. 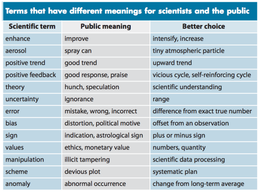 Sommerville and Hassol, 2011 Sommerville and Hassol, 2011 So I've decided to write a blog. Why? Well as much as I love scientific writing, I also have views and opinions that I'm keen to to express in a different format, and a blog seems like a great outlet to do so. I think a major current issue relates to what myself and others call the 'science-public disconnect'; a term that describes the gap between what scientists say and what the public hears. This disconnect is caused when scientific findings are twisted or so hyped up by the media that the essence (and limitations) of the scientific finding is lost and the public is left with a message that differs greatly from that which was intended. Obviously media outlets want headlines and hits, but exaggeration and glossing over the finer details can often do more harm than good by leading to an increase in the public mistrust of science and medicine. One way I think that this can be remedied is by scientists themselves communicating with the lay public to explain their research, and provide insight into their research environment. This is one of the things I intend to do with this blog. So I'll be writing about my own research, my research field more broadly and my thoughts on a number of related issues such as my perspective on what its like to be an an early career researcher in an increasingly competitive and insecure environment, and what its like to split myself into many parts - including a researcher, a wife and a (new) mother. So who am I?My bio provides a brief outline of who I am and what I do, but in brief I'm a research scientist studying the brain and behaviour in severe psychiatric disorders. I'm mainly interested in understanding cognitive (thinking) skills including that related to social perception and emotion regulation. I work at the Melbourne Neuropsychiatry Centre (MNC) in Melbourne, Australia. MNC is a centre of the Department of Psychiatry at the University of Melbourne, headed by Prof Christos Pantelis. It has an international reputation in the areas of cognition and brain changes in schizophrenia and related disorders, with several significant papers emerging from the group in journals such as Nature, JAMA Psychiatry, PNAS and Schizophrenia Bulletin. It is home to several very talented researchers including Dr Vanessa Cropley, A/Prof Sarah Whittle, A/Prof Ben Harrison, Dr Andrew Zalesky, Dr Chad Bousman and Dr Julian Simmons.  Rossell group in Florence, 2016 Rossell group in Florence, 2016 I'm also part of the Centre for Mental Health at Swinburne University and the Cognitive Neuropsychiatry group at the Monash Alfred Psychiatry Research Centre, headed by Prof Susan Rossell. This group is focussed on characterising cognitive patterns and understanding the neurobiology of cognitive symptoms in psychosis and related disorders through neurobehavioural, neuroimaging and genetic techniques.
|
Tamsyn Van RheenenNHMRC Peter Doherty Biomedical Research Fellow ArchivesCategories |



 RSS Feed
RSS Feed